Expanded Access to Unapproved Drugs, Biologics, or Devices
Book search
Expanded Access to Unapproved Drugs or Biologics
Under FDA regulations (21 CFR 312.300), expanded access allows for the use of unapproved drugs and biologics outside of a clinical trial for patients with serious diseases or conditions when there is no satisfactory alternative therapy to treat the patient’s disease or condition. This is sometimes referred to as compassionate use or treatment use. While expanded access is not considered a clinical investigation, FDA submission and IRB review are required.
Key Definitions:
Immediately life-threatening disease or condition means a stage of disease in which there is reasonable likelihood that death will occur within a matter of months or in which premature death is likely without early treatment.
Serious disease or condition means a disease or condition associated with morbidity that has substantial impact on day-to-day functioning. Short-lived and self-limiting morbidity will usually not be sufficient, but the morbidity need not be irreversible, provided it is persistent or recurrent. Whether a disease or condition is serious is a matter of clinical judgment, based on its impact on such factors as survival, day-to-day functioning, or the likelihood that the disease, if left untreated, will progress from a less severe condition to a more serious one.
Criteria for all expanded access uses for drugs and biologics:
The FDA must determine that:
(1) The patient or patients to be treated have a serious or immediately life-threatening disease or condition, and there is no comparable or satisfactory alternative therapy to diagnose, monitor, or treat the disease or condition;
(2) The potential patient benefit justifies the potential risks of the treatment use and those potential risks are not unreasonable in the context of the disease or condition to be treated; and
(3) Providing the investigational drug for the requested use will not interfere with the initiation, conduct, or completion of clinical investigations that could support marketing approval of the expanded access use or otherwise compromise the potential development of the expanded access use.
Types of expanded access for drugs and biologics
Under FDA’s current regulations, there are three categories of expanded access as shown in the diagram below.
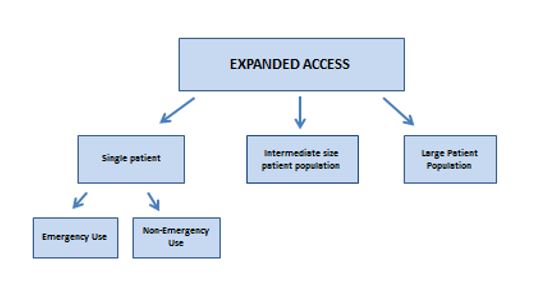
Single patient expanded access, non- emergency use
In addition to the criteria for all expanded access uses listed above, the following must also be met:
- The physician must determine that the probable risk to the person from the investigational drug is not greater than the probable risk from the disease or condition; and
- FDA must determine that the patient cannot obtain the drug under another IND or protocol.
If the drug is the subject of an existing IND, the expanded access IND submission may be made by the sponsor or by a licensed physician. Per the agreement between the University of Pittsburgh and UPMC, if the expanded access IND is industry sponsored, the expanded access protocol does not fall under the authority of the University of Pittsburgh IRB and must be processed through the UPMC OSPARS office. If the expanded access IND is investigator initiated, it will be processed through the University of Pittsburgh IRB, and if there is an agreement for the provision of the drug, that agreement will be processed via UPMC OSPARS.
Procedures for IRB submission of single patient, non-emergency expanded access protocols
Single patient, non-emergency expanded access protocols must be submitted through PittPRO and require IRB review and approval under FDA regulations. HRP is cognizant of the need for timely review for these cases and will make every effort to assign these cases to the first available meeting with expertise. The treating physician may complete the Form FDA 3926, which is a streamlined process created specifically for single patient IND submissions, allowing for IRB Chairperson concurrence rather than a full board meeting. Please see the IND and IDE Support (IIS) website for information about preparing an IND submission to FDA.
Single Patient Expanded Access, emergency use
If there is an emergency that requires a patient to be treated before a written IND submission can be made to FDA, an emergency IND may be granted by FDA. Under the emergency use provisions in the FDA regulations (21 CFR 56.104(c)), the emergency use of an unapproved drug is an exemption from prior review and approval by the IRB, but must be reported to the IRB. According to FDA regulations (21 CFR 56.102(d), emergency use is the use of a test article on a patient in a life-threatening situation in which no standard acceptable treatment is available, and in which there is not sufficient time to obtain IRB approval. Life-threatening, for the purposes of section 56.102(d), includes the scope of both life-threatening and severely debilitating, as defined below.
- Life-threatening means diseases or conditions where the likelihood of death is high unless the course of the disease is interrupted and diseases or conditions with potentially fatal outcomes, where the end point of clinical trial analysis is survival. The criteria for life-threatening do not require the condition to be immediately life-threatening or to immediately result in death. Rather, the patients must be in a life-threatening situation requiring intervention before review at a convened meeting of the IRB is feasible.
- Severely debilitating means diseases or conditions that cause major irreversible morbidity. Examples of severely debilitating conditions include blindness, loss of arm, leg, hand or foot, loss of hearing, paralysis or stroke.
The emergency exemption from prospective IRB review allows for one emergency use of a drug or biologic without prospective IRB review. FDA regulations require that any subsequent use of the investigational product at the institution have prospective IRB review and approval. However, in guidance documents, FDA acknowledges that it would be inappropriate to deny emergency treatment to a second individual if the only obstacle is that the IRB has not had sufficient time to convene a meeting to review the protocol.
Procedures for IRB submission of single patient, emergency use protocols
The University of Pittsburgh HRP requires that, when possible, the IRB be notified in advance of the proposed emergency use of an unapproved drug or biologic. IRB notification is done through the Emergency Use pathway in PittPRO. The EU pathway provides a mechanism for verifying that the intended use meets criteria, and uploading documentation of correspondence with FDA, including the Form FDA 3926, emergency IND approval, the treatment plan and the proposed consent form. The IRB Chair or Vice Chair will review and concur with the emergency use. The EU pathway also allows for submission of follow up information on the status of the patient. Please note that concurence of the emergency use by the IRB Chair or Vice Chair should not be construed as IRB approval. Only proposals that undergo full IRB review can receive IRB approval.
In the event of a waiver of informed consent for an emergency use, the IRB Chair or Vice Chair will confirm that both the physician holding the emergency IND and a physician who is not otherwise participating in the emergency use have certified in writing all of the following:
- the patient is confronted by a life-threatening situation necessitating use of the test article;informed consent cannot be obtained because of an inability to communicate with, or obtain legally effective consent from, the patient;
- time is not sufficient to obtain consent from the patient’s legal representative;
- no alternative method of approved or generally recognized therapy is available that provides an equal or greater likelihood of saving the patient’s life;
If, in the physician’s opinion, there is not sufficient time to obtain an independent physician’s determination that the four criteria are met, the physician holding the emergency IND should make the determination and subsequently obtain (i.e., within five working days) a review of his/her determination by a physician not participating in the emergency treatment.
Expanded Access for Intermediate-size populations
FDA may permit an investigational drug to be used for treatment of a patient population smaller than that typical of a treatment IND or treatment protocol. In cases where FDA has received a significant number of requests for individual patient expanded access for the same use, a sponsor may be asked to consolidate expanded access under this category.
In addition to the criteria listed at the beginning of this section for all expanded access, the FDA must also determine that there is enough evidence that the drug is safe at the proposed dose and duration and there is at least preliminary evidence of effectiveness of the drug as a therapeutic option in the patient population. For more information about FDA requirements, please see 21 CFR 312.315.
Procedures for IRB submission of expanded access protocols for intermediate–size populations
Intermediate size expanded access protocols must be submitted through usual procedures in PittPRO and require full IRB review and approval under FDA regulations. Please see the IND and IDE Support (IIS) website for information about preparing an IND submission to FDA.
Expanded Access for Large Patient Populations
Expanded access protocols for large patient populations are also referred to as treatment IND or treatment protocols and are usually sponsored by a pharmaceutical company. This category is used for widespread treatment use of an investigational drug. In addition to the criteria listed at the beginning of this section for all expanded access, FDA must also determine that the drug is being investigated in a controlled trial under an IND to support a marketing application for the expanded access or all clinical trials of the drug have been completed, the sponsor is actively pursuing marketing for approval of the expanded access and there is sufficient data supporting safety and effectiveness of the drug for the expanded access.
Procedures for IRB submission of expanded access protocols for large patient populations
Expanded access protocols for large patient populations must be submitted per usual procedures through PittPRO and require full IRB review and approval under FDA regulations.
Expanded Access to Unapproved Devices
According to FDA regulations, an unapproved medical device may normally only be used on human subjects through an approved clinical study in which the subjects meet certain criteria and the device is only used in accordance with the approved protocol by a clinical investigator participating in the clinical trial. However, FDA recognizes that there may be circumstances under which a health care provider may wish to use an unapproved device to save the life of a patient or to help a patient suffering from a serious disease or condition for which there no other alternative therapy exists. This is sometimes referred to as compassionate use or treatment use.Patients/physicians faced with these circumstances may request access to investigational devices under one of the following mechanisms by which FDA may make an unapproved device available.
Key Definitions:
Unapproved medical device is a device that is utilized for a purpose, condition, or use for which the device requires, but does not have, an approved application for premarket approval under section 515 of the Federal Food, Drug, and Cosmetic Act (21 U.S.C. 360e)(the act) or an approved IDE under section 520(g) of the act (21 U.S.C. 360j(g)).
IDE - An approved investigational device exemption permits a device that otherwise would be required to comply with a performance standard or to have premarket approval to be shipped lawfully for the purpose of conducting investigations of that device.
Emergency Use of an unapproved device
As mentioned above, an unapproved device should normally only be used in human subjects if it is approved for clinical testing under an IDE and if it is used by an investigator for the sponsor in accordance with the terms and conditions of the application. Emergency use of an unapproved device, however, may also occur when: (i) an IDE for the device does not exist, (ii) when a physician wants to use the device in a way not approved under the IDE, or (iii) when a physician is not an investigator under the IDE. The sponsor must notify the FDA within 5 days through submission of an IDE report describing the case and the patient protection measures that were followed.
Life-threatening, for the purposes of section 56.102(d), includes the scope of both life-threatening and severely debilitating, as defined below.
- Life-threatening means diseases or conditions where the likelihood of death is high unless the course of the disease is interrupted and diseases or conditions with potentially fatal outcomes, where the end point of clinical trial analysis is survival. The criteria for life-threatening do not require the condition to be immediately life-threatening or to immediately result in death. Rather, the patients must be in a life-threatening situation requiring intervention before review at a convened meeting of the IRB is feasible.
- Severely debilitating means diseases or conditions that cause major irreversible morbidity. Examples of severely debilitating conditions include blindness, loss of arm, leg, hand or foot, loss of hearing, paralysis or stroke.
Criteria: The physician who intends to use the device must determine that the following criteria are met
- Life-threatening or serious disease or condition that needs immediate treatment
- No generally acceptable alternative treatment for the condition exists
- Because of the immediate need to use the device, there is no time to obtain FDA approval
FDA expects the physician to make the determination that the patient’s circumstances meet the above criteria, to assess the potential for benefit from the use of the unapproved device and to have substantial reason to believe that benefits will exist.
Under the emergency use provisions in the FDA regulations (21 CFR 56.104(c)), the emergency use of an unapproved test article is an exemption from prior review and approval by the IRB, but must be reported to the IRB within 5 working days. FDA guidance indicates that the physician should follow as many patient protection procedures as possible, including:
- Informed consent from the patient or a legal representative
- Clearance from the institution as specified by their policies
- Concurrence of the IRB Chairperson
- An independent assessment from an uninvolved physician; and
- Authorization from the device manufacturer.
Procedures for IRB submission of protocols for emergency use of unapproved devices
The University of Pittsburgh HRP requires that, when possible, the IRB be notified in advance of the proposed emergency use of an unapproved device. IRB notification is done through the Emergency Use pathway in PttPRO. The EU pathway provides a mechanism for verifying that the intended use meets criteria and, uploading documentation of correspondence with FDA, the proposed treatment plan, and the proposed consent form. The IRB Chair or Vice Chair will review and concur that the emergency use meets the criteria. The EU pathway also allows for submission of follow up information on the status of the patient. Please note that concurrence of the emergency use by the IRB Chair or Vice Chair should not be construed as IRB approval. Only proposals that undergo full IRB review can receive IRB approval.
In the event of a waiver of informed consent for an emergency use, the IRB Chair or Vice Chair will confirm that both the investigator and a physician who is not otherwise participating in the clinical investigation have certified in writing all of the following:
- the patient is confronted by a life-threatening situation necessitating use of the test article;
- informed consent cannot be obtained because of an inability to communicate with, or obtain legally effective consent from, the patient;
- time is not sufficient to obtain consent from the patient’s legal representative;
- no alternative method of approved or generally recognized therapy is available that provides an equal or greater likelihood of saving the patient’s life;
If, in the investigator’s opinion, there is not sufficient time to obtain an independent physician’s determination that the four criteria are met, the investigator should make the determination and subsequently obtain (i.e., within five working days) a review of his/her determination by a physician not participating in the investigation.
Expanded Access (or Single Patient/Small Group Access)
FDA’s expanded access provision is designed to provide access to an investigational device for patients who are not eligible for the clinical trial but for whom the treating physician believes the device may provide a benefit in treating and/or diagnosing their disease or condition. Expanded access use may be used only during the clinical trial for which the device is being tested. Expanded access may be approved for a single patient or a small group of patients.
Criteria:
- The device is intended to treat or diagnose a serious disease or condition
- There is no comparable or satisfactory alternative device or therapy available
Prior FDA approval is required before expanded access occurs. The sponsor of the IDE is required to submit an IDE supplement requesting approval under 812.35(a) in order to treat the patient. For further instructions about FDA requirements for the IDE supplement, please refer to the FDA website.
The physician may not treat the patient identified in the IDE supplement until FDA approves the expanded access for the intended patient. FDA will consider preliminary evidence of safety and effectiveness as well as whether the expanded access would interfere with the conduct of a clinical trial to support marketing approval. Once approved, the patient should be monitored for safety. Follow up information on the use of the device should be submitted in an IDE Report after expanded access has ended.
Procedures for IRB submission of protocols for expanded access of unapproved devices
For investigator initiated IDEs, expanded access h protocols must be submitted through the usual procedures in PittPRO. Refer to the IIS website for this type of application. Per the agreement between the University of Pittsburgh and UPMC, if the IDE is industry sponsored, the expanded access protocol does not fall under the authority of the University of Pittsburgh IRB and must be processed through the OSPARS office. If the IDE is investigator initiated, it will be processed through the University of Pittsburgh IRB, and if there is an agreement for the provision of the device, that agreement will be processed via UPMC OSPARS.
Treatment Use of Investigational Devices
These procedures are intended to facilitate the availability of devices that are not FDA approved for marketing, but are under clinical investigation for a serious or immediately life threatening disease or condition in patients for whom there is no comparable or satisfactory alternative device or treatment available. During the trial or prior to final FDA action on the marketing approval, it may be appropriate to use the device to treat patients not in the trial under treatment IDE regulations (21 CFR 812.36).
For the purposes of treatment use, immediately life-threatening disease means a stage of a disease in which there is reasonable likelihood that death will occur within a matter of months or in which premature death is likely without early treatment.
Criteria:
- The device is intended to treat or diagnose a serious or immediately life-threatening disease or condition;
- There is no comparable or satisfactory alternative device or other therapy available to treat or diagnose that stage of the disease or condition in the intended patient population;
- The device is under investigation in a controlled clinical trial for the same use under an approved IDE, or such clinical trials have been completed; and
- The sponsor of the investigation is actively pursuing marketing approval/clearance of the investigational device with due diligence.
A treatment IDE application must be submitted to FDA and approval must be obtained prospectively. For information about FDA requirements for submission of a treatment IDE application, please see the FDA Expanded Access page.
Procedures for IRB submission of protocols for treatment use of unapproved devices
For investigator-initiated treatment IDEs, treatment use protocols must be submitted through the usual procedures in PittPRO. Per the agreement between the University of Pittsburgh and UPMC, if the treatment IDE is industry sponsored, the expanded access protocol does not fall under the authority of the IRB and must be processed through the OSPARS office. If the treatment IDE is investigator initiated, it will be processed through the IRB, and if there is an agreement for the provision of the device, that agreement will be processed via UPMC OSPARS.
References
21CFR 312.300
21 CFR 56.102
21 CFR 812
FDA Guidance on Expanded Access for Medical Devices
5/19/2021
